Written by Lisa Eramo
Key takeaways
- Revenue cycle management spans 8 stages, from patient registration to denial management, and each one directly affects your practice’s cash flow.
- Tracking KPIs like days in accounts receivable (A/R), denial rate, and net collection rate gives you real-time visibility into financial performance.
- Technology and automation — including EHR integration and real-time insurance verification — reduce manual errors and streamline billing processes.
- Deciding whether to optimize in-house, outsource, or adopt a hybrid RCM model depends on your staffing, denial rates, and practice volume.
Revenue cycle management (RCM) is the financial process that tracks every dollar from the moment a patient schedules an appointment to the final payment posting. It covers patient registration, insurance verification, medical coding, claim submission, payment collection, and denial follow-up. For private practices, RCM is the financial backbone that keeps operations running and cash flow steady.
This guide walks through the full revenue cycle lifecycle — all 8 stages — along with the key metrics that measure performance, common areas where revenue leaks happen, and strategies to optimize every step. Whether your practice handles billing in-house or is considering outsourcing, understanding how RCM works end to end will help you protect your bottom line, reduce claim denials, and improve your overall financial health.
Why RCM matters for private practices
Private practices operate on thinner margins than large health systems, which makes every dollar of reimbursement count. Several forces are putting more pressure on practice finances than ever before:
- Rising patient financial responsibility. Higher deductibles and co-pays are shifting a larger share of financial responsibility to patients.
- Stagnant payer reimbursement rates. Nominal payment increases do not keep pace with rising costs.
- Compliance risk. Regulatory changes around billing and coding require constant attention, and mistakes can trigger audits or penalties.
- Staffing challenges. It is harder than ever to keep experienced billing professionals on the team, leading to errors that create lost revenue.
Strong RCM protects a practice’s financial stability by keeping patient payments flowing, reducing claim rejections, and catching problems early. It also supports a better patient experience — clear billing statements and fewer surprise balances build trust.
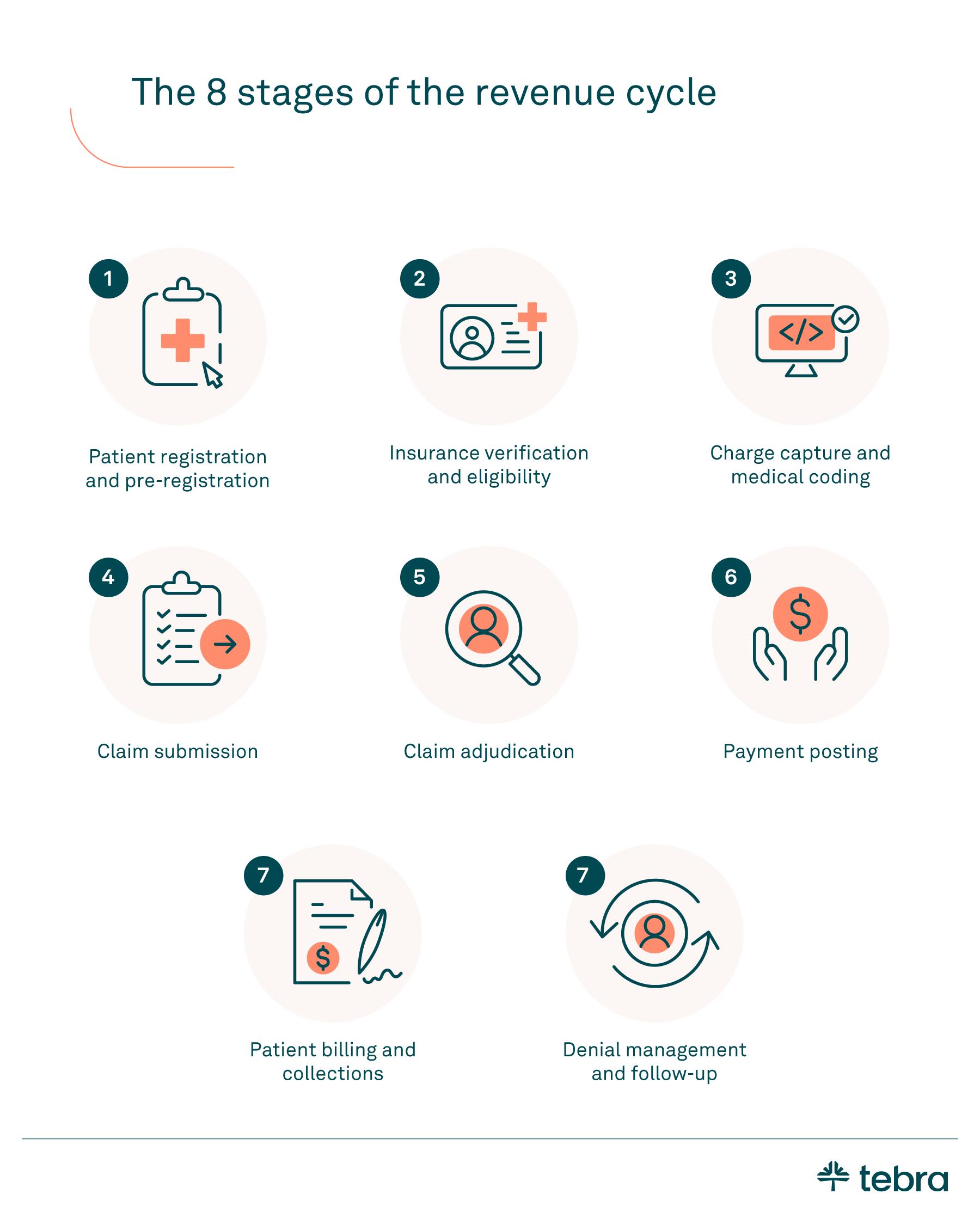
The 8 stages of the revenue cycle
The revenue cycle is an end-to-end process that begins before a patient ever walks through the door and continues long after the visit ends. Each stage builds on the one before it, so accuracy at every step matters.
1. Patient registration
Patient registration is the front-end starting point of the revenue cycle. During this step, staff collect patient information (including demographics, contact details, and insurance information) either before the visit or at check-in.
Accurate data capture at this stage prevents downstream errors that cascade through the entire billing process. A misspelled name, outdated insurance ID, or wrong date of birth can result in a denied claim days or weeks later. Standardized intake forms and verification workflows help front-desk teams get it right the first time.
2. Insurance verification and eligibility
Once patient registration is complete—and before services are rendered—staff should verify insurance coverage to determine the patient’s eligibility for the planned services. This includes checking benefits, reviewing coverage limitations, and identifying any prior authorization requirements.
Real-time eligibility checks reduce claim denials by catching coverage gaps before they become billing problems. When a patient’s insurance has lapsed, or a procedure requires prior authorization, the practice can address it up front rather than chasing a rejection after services are rendered.
Insurance companies update their rules frequently, so verifying coverage and eligibility at every visit — and for every patient — is a best practice.
3. Charge capture and medical coding
After a patient visit, providers document the services they performed. Medical coders then translate that clinical documentation into standardized CPT, ICD-10, and HCPCS codes that payers use to process claims.
Accuracy is essential — coding errors are one of the top causes of claim denials. Undercoding leaves money on the table, while overcoding can trigger audits and compliance issues. Regular coding audits help practices catch patterns of inaccuracy before they become systemic problems. The connection between thorough clinical documentation and accurate billing cannot be overstated.
4. Claim submission
Once coding is complete, the practice submits each claim electronically using their EHR system. They submit claims either directly to payers or through a clearinghouse. The goal at this stage is to submit clean claims — meaning claims that contain all required information, have no errors, and can be processed without additional follow-up.
Every claim that requires rework costs time and delays reimbursement. A strong claims processing workflow includes automated scrubbing tools that flag errors before submission and reduce the volume of rejections that billing staff must handle manually.
5. Claim adjudication
Claim adjudication happens on the payer side. The insurance company reviews the submitted claim, verifies the patient’s coverage, applies contractual adjustments, and decides whether to approve the payment, deny the payment, or request additional information.
This stage is largely outside the practice’s direct control. However, the quality of work done in earlier stages — accurate patient information, verified eligibility, correct coding — directly influences whether insurance claims move through adjudication smoothly or get flagged. Health plans each have their own processing rules and timelines, delayed payer responses at this stage are not always a reflection of a billing error.
6. Payment posting
When the practice receives an insurance payment, staff post it to the applicable patient’s account. This step is more than bookkeeping — it is an active reconciliation process.
Staff compare the actual payment received to the expected reimbursement based on the payer contract. This is where underpayments and discrepancies may surface. If a payer reimburses less than the contracted rate, the practice needs to identify the shortfall and follow up with the payer to determine the reason for the underpayment. For example, it could be due to an error with the fee schedule loaded on the payer’s (or provider’s) side.
However, it could also be due to system configuration issues, perceived documentation gaps, or a whole host of other reasons. Determining the root causes of underpayments and posting all payments consistently keeps accounts receivable —and financial reports—accurate.
7. Patient billing and collections
After insurance pays its portion, any remaining balance — including co-pays, deductibles, and other patient financial responsibility — gets billed to the patient. Patient payments represent a growing share of practice revenue, making this stage more important than it was a decade ago.
Clear, easy-to-read statements reduce confusion and speed up collections. Offering payment plans and multiple payment options (online portal, credit card, phone) helps patients manage their medical billing obligations. Practices that communicate financial responsibility up front, ideally before the visit or at the point of care, tend to collect more and faster.
8. Denial management and follow-up
Denial management is the back-end process of identifying denied claims, investigating root causes, preparing appeals, and resubmitting corrected claims. Many practices leave significant money on the table by not working denials aggressively.
Tracking denial patterns over time is where the real value lies. If a specific payer consistently denies claims for a particular reason, or if a certain code triggers frequent rejections, those patterns reveal fixable process gaps. A structured follow-up workflow — with assigned ownership, deadlines, and escalation paths — turns denial management from a reactive scramble into a proactive revenue recovery function.
Key RCM metrics and KPIs
Benchmarking and tracking the right key performance indicators gives practice leaders a clear view of where the revenue cycle is performing well and where it needs attention. The following metrics are the most widely used:
- Days in A/R. Average number of days it takes to collect payment after a claim is submitted
- Clean claim rate. Percentage of claims accepted on first submission without errors
- Denial rate. Percentage of submitted claims payers reject or don’t pay
- Net collection rate. Percentage of allowed reimbursement collected after contractual adjustments
- Patient balance resolution time. Average number of days it takes to fully collect or resolve a patient’s financial responsibility from the date the balance is first billed
- Bad debt percentage. Percentage of patient balances written off as uncollectable
These metrics work best when tracked over time rather than as one-time snapshots. Monitoring trends in accounts receivable, clean claim rates, and denied claims month over month helps practices spot problems early and measure the financial performance impact of any process changes they make. Consistent KPI tracking turns cash flow management from guesswork into a data-driven discipline.
Common RCM challenges and where revenue leaks occur
Even well-run practices face recurring challenges that erode revenue. The following are the most common areas where revenue leaks occur:
- Front-end data entry errors. Incorrect or incomplete patient information at registration leads to claim rejections that could have been prevented with better intake workflows.
- Medical coding inaccuracies. Undercoding, overcoding, and mismatched diagnosis and procedure codes are among the top drivers of claim denials and audit risk.
- Payer variability and changing reimbursement rules. Each insurance company has its own requirements, and those rules shift frequently, creating discrepancies between what practices expect and what they receive.
- Patient collections and growing patient financial responsibility. As deductibles rise, practices must collect more of the balance owed directly from patients — a process many are not staffed or equipped to handle well.
- Administrative burdens and staff burnout. Manual billing processes, high claim volumes, and constant follow-up overwhelm teams, leading to errors and lost revenue over time.
- Lack of follow-up on denied claims. Practices that do not have a structured denial management process often write off recoverable revenue simply because no one worked the claim.
How technology and automation improve RCM
When applied to the right stages of the billing process, automation reduces manual work, catches errors earlier, and accelerates reimbursement. The goal is not to replace human judgment but to free up staff for higher-value tasks.
Where automation makes the biggest impact
Several areas of the revenue cycle benefit most from automation:
- EHR integration. Connecting electronic health records directly to billing and coding workflows reduces duplicate data entry and keeps patient information consistent across systems.
- Real-time insurance verification. Automated eligibility checks at the time of registration or upon check-in flag coverage issues before services are rendered, cutting down on preventable denials.
- Automated charge capture. Extracting charges directly from clinical documentation reduces missed charges and speeds up the coding-to-claim submission timeline.
- RCM software and practice management platforms. These tools combine claim scrubbing, submission tracking, payment posting, and denial workflows into a single system, giving staff a unified view of the revenue cycle.
Where artificial intelligence fits in
Artificial intelligence is beginning to impact advanced RCM functions in several key ways:
- Claim denial prediction. Predictive models can flag claims prior to submission when those claims are likely to be denied, giving billing teams time to correct issues proactively.
- Documentation review. AI-powered coding tools compare documentation against submitted codes to catch discrepancies.
- Claims management analysis. These tools detect trends across thousands of claims, surfacing payer-specific denial patterns or coding errors that would take a human analyst much longer to find.
Where humans are still critical
Despite advances in automation and AI, human expertise remains critical in several areas of the billing process:
- Complex appeals. Nuanced clinical scenarios still require experienced billing professionals to review and respond appropriately to denials.
- Patient communication. Explaining balances, setting up payment plans, and managing sensitive financial conversations benefit from empathy and personal attention.
- Compliance oversight. Human judgment is necessary to interpret regulatory changes and apply them correctly to specific billing scenarios.
- Payer negotiations. Relationship-building and strategic thinking around contract terms and reimbursement rates depend on human involvement.
When to optimize, outsource, or automate your RCM
Not every practice needs the same RCM approach. The right model—optimize in-house operations, outsource completely, or pursue a hybrid approach—depends on your team’s capacity, your denial rates, and the complexity of your payer mix.
Optimizing in-house RCM
Keeping RCM in-house works best for practices with experienced billing teams and manageable claim volumes. With this model, the focus should be on refining workflows, investing in staff training, and upgrading technology to reduce manual processes.
In-house optimization gives healthcare organizations full control over every stage of the revenue cycle. The trade-off is that it requires ongoing investment in people and tools, and it can be hard to scale during periods of rapid growth.
Outsourcing RCM
Outsourcing is worth considering when a practice struggles with chronic staffing shortages, consistently high denial rates, or an inability to ramp up during times of rapid patient volume growth. Third-party RCM providers bring specialized expertise and technology that can improve operational efficiency.
The trade-offs are real, though. Outsourcing involves cost — typically a percentage of collections — and you give up some direct control over billing processes. Data access and reporting transparency vary by vendor, so practices should evaluate these factors carefully before signing a contract.
Hybrid RCM models
A hybrid approach keeps some RCM functions in-house while outsourcing others. For example, a practice might handle patient registration and payment posting internally but outsource complex medical coding and claims management to a specialized partner.
This model is increasingly common among mid-sized practices that want to maintain control over patient-facing billing functions while offloading the most technical or time-consuming work to an outsource partner. Hybrid models offer flexibility, though they require clear communication and defined handoff points between internal staff and external medical billing partners.
RCM best practices by role
Strong revenue cycle performance is not the billing department’s job alone. Every team member plays a part in keeping revenue flowing. Consider each of the following critical roles and their respective responsibilities:
- Front office. Collect accurate patient registration data, run real-time eligibility checks, and communicate financial responsibility to patients before their visit or at the time of service.
- Clinicians. Provide thorough, specific clinical documentation that supports accurate medical coding and reduces the risk of downcoding or denials.
- Billing team. Focus on clean claim submission, track denial patterns, follow up on rejected claims within defined timelines, and maintain payer-specific knowledge.
- Practice leadership. Monitor KPIs regularly, invest in technology and training, evaluate whether current RCM workflows meet financial targets, and make staffing decisions based on data rather than assumptions.
Strengthen your revenue cycle, strengthen your practice
Revenue cycle management is a full-cycle process, and every stage — from patient registration through denial management — directly impacts your practice’s cash flow and financial performance. There are no shortcuts. Weak links at any point in the cycle create downstream problems that cost time and money.
Medical practices that perform best financially are ones that track their KPIs consistently, address denial patterns proactively, and invest in the right combination of people, processes, and technology. Whether you choose to optimize your in-house team, outsource to a specialized partner, or build a hybrid model, the key is treating RCM as a strategic priority rather than an administrative afterthought.
If your practice is ready to strengthen its revenue cycle, start by auditing your current metrics — especially your clean claim rate, denial rate, and days in A/R. From there, identify the stages where you are losing the most revenue and focus your improvements there.
Ready to improve collections and reduce denials? Learn how Tebra’s managed billing services can help your practice get paid faster.