Practice management
Tebra makes it easy to successfully manage your medical billing and get paid faster.
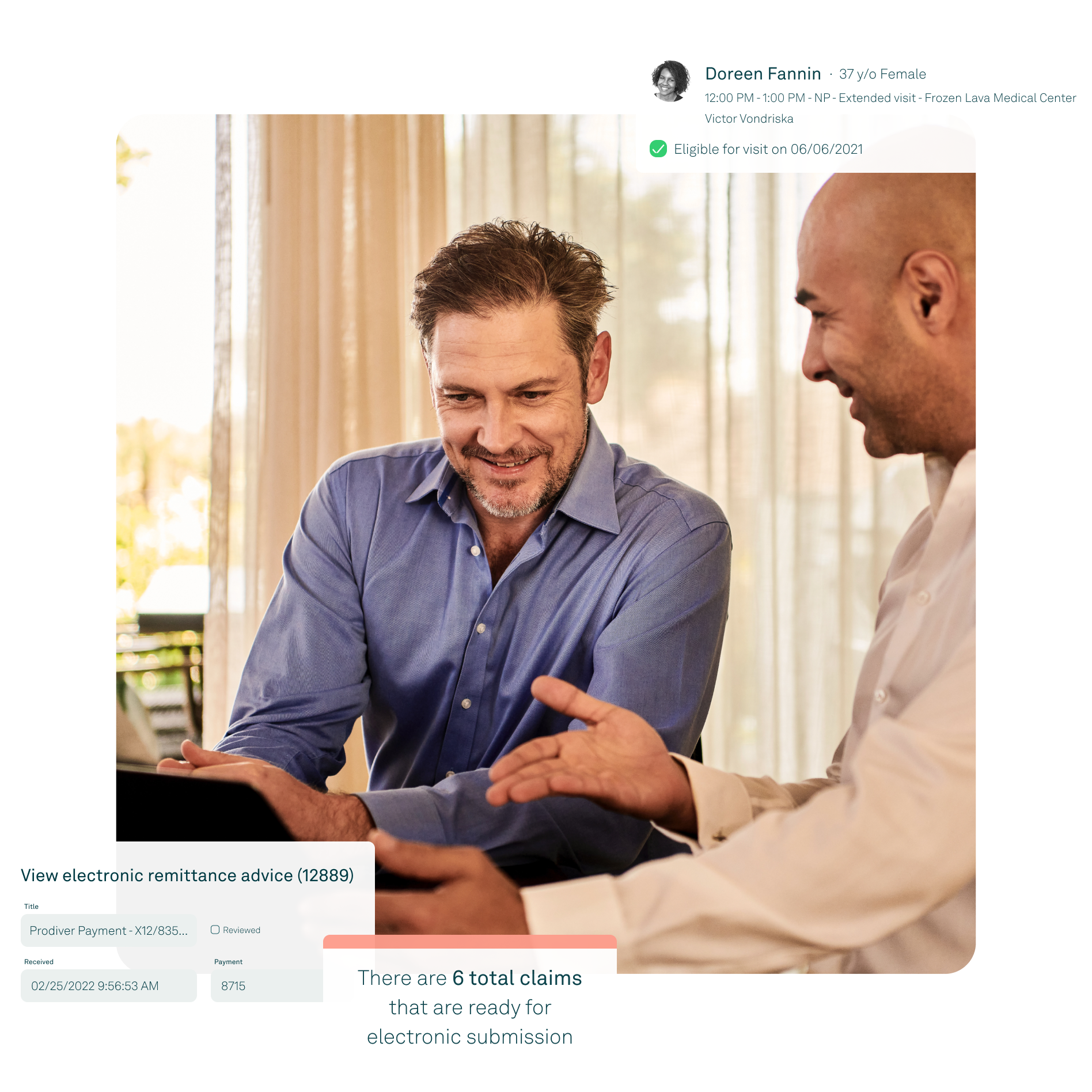
Streamline medical billing complexities for better practice management
Simplify billing and maintain control of your practice by automating processes to get paid faster. Tebra helps you easily manage the complications that come with medical billing so you can concentrate on patient care. Flexible workflows, A/R management, and reporting and analytics give you total visibility into your practice’s financial health.
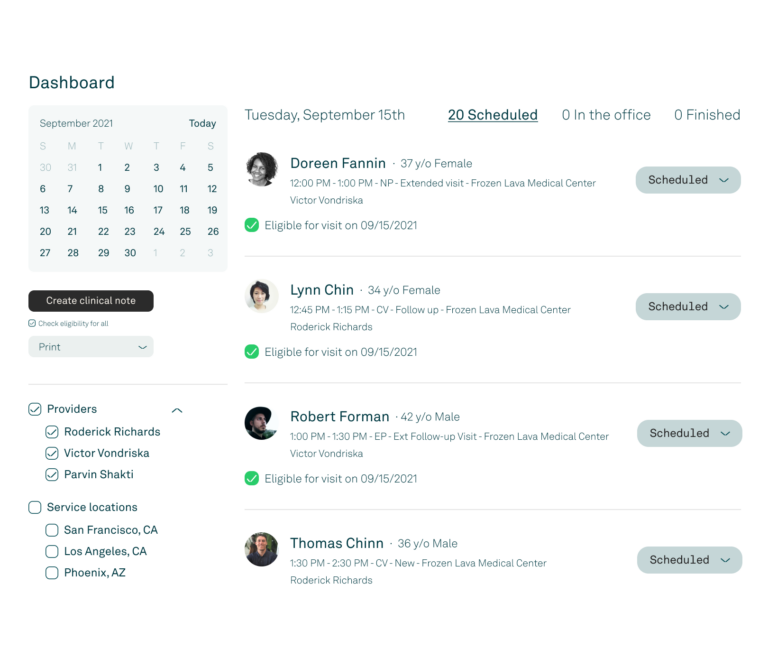
KPI and workflow dashboard
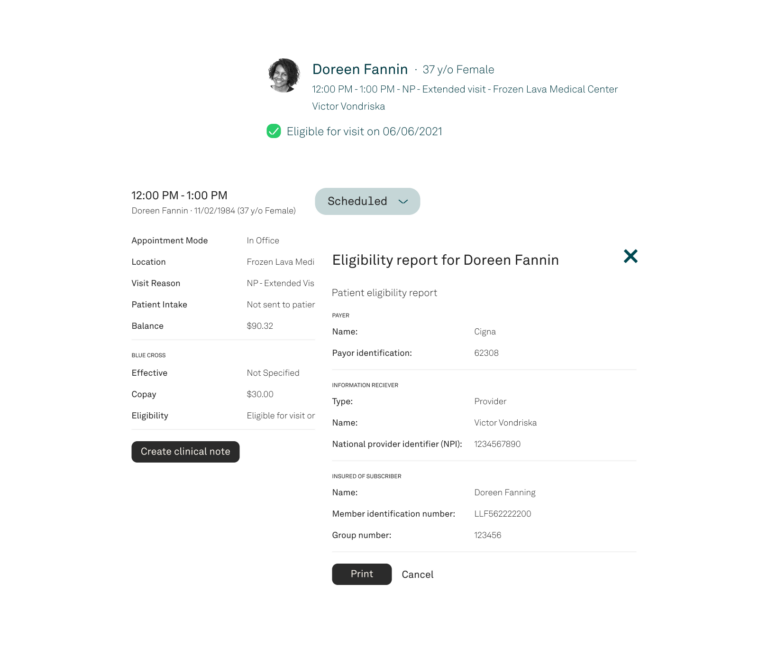
Eligibility checks and patient authorizations
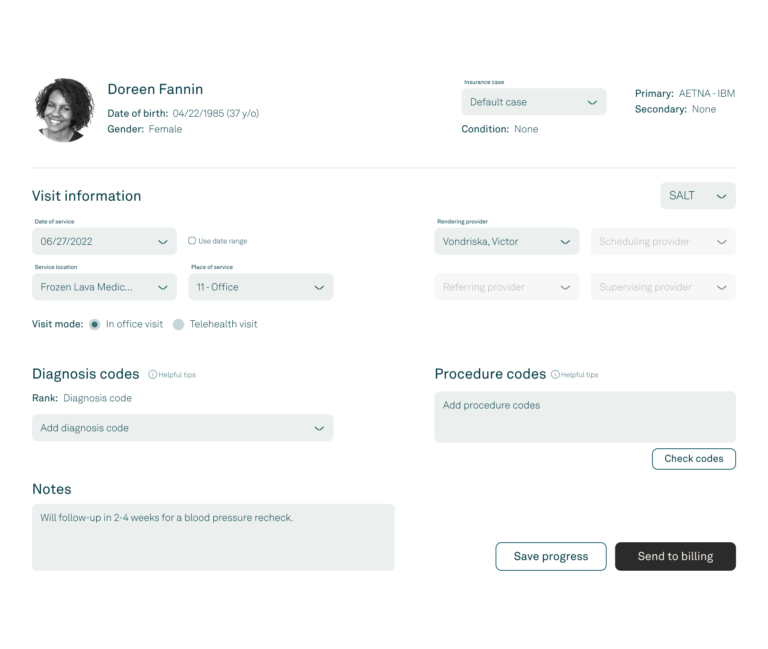
Charge capture and encounter review
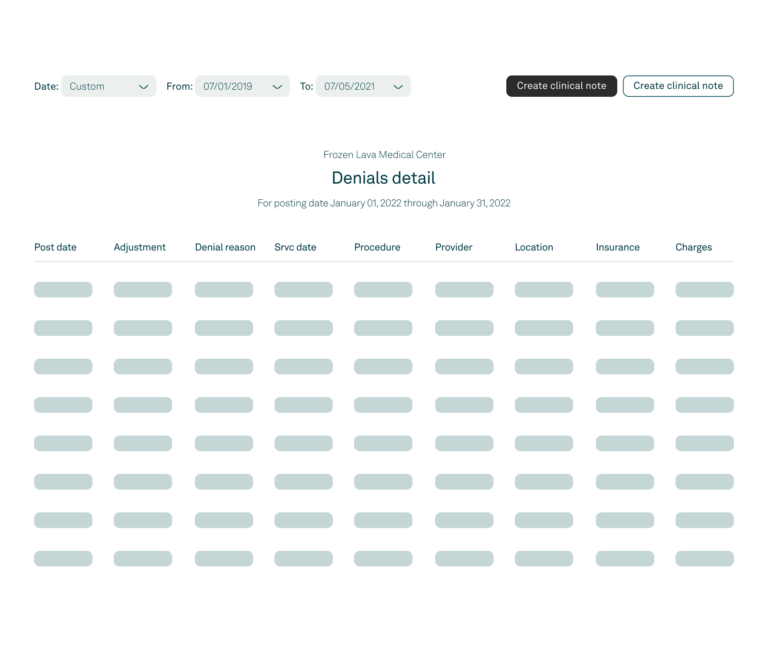
Rejection and denial management
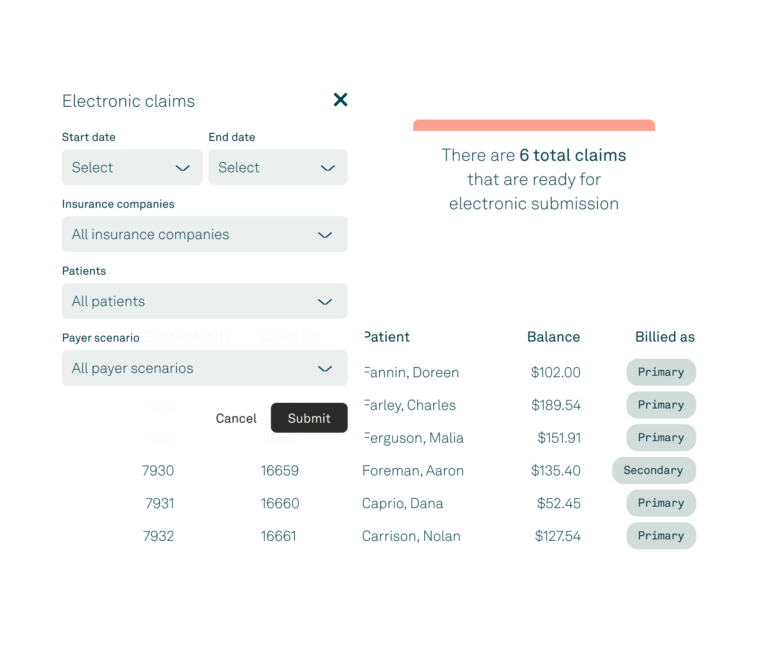
Claim submissions

Electronic remittance advice (ERA)
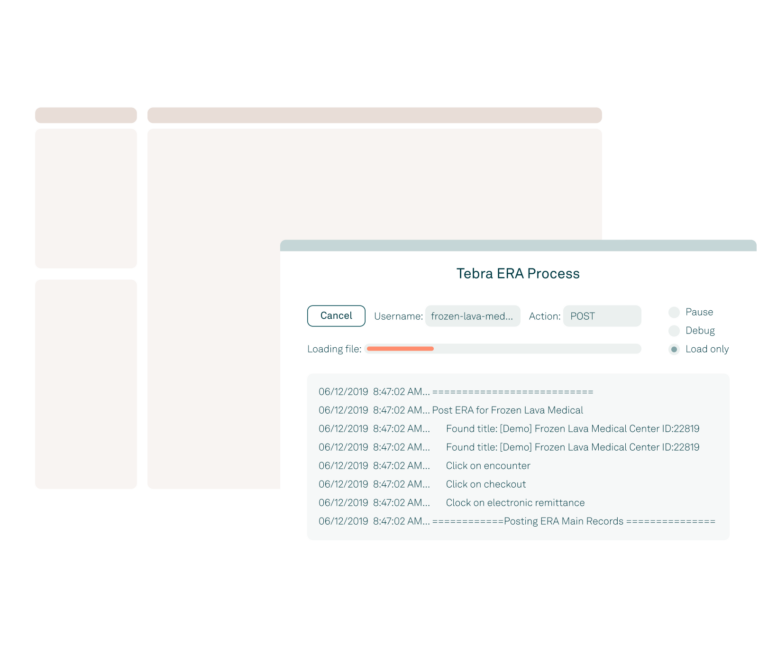
Robotic process automation (RPA)
Experience Tebra’s complete operating system
-
Tebra has given me a way to look at all my clients at an enterprise level and to provide our independent practices the stability and accountability they need to succeed.”Josh Santillan, Chief Operations OfficerMedical Billing Unlimited
-
Tebra allows us to improve our clients’ processes. If we make our clients more efficient, then we’re more efficient and we can help them grow, and that’s the path to success for Medical Claims Billing.”Josh Santillan, Chief Operations OfficerMedical Billing Unlimited
-
They are so responsive and have great follow-through. Using Tebra, we’ve gotten to a a place where we have very few errors, our claims are clean, and we get paid quickly.”Theresa JenkinsAppalachia Medical Clinic
Resources
-
 Case study
Case studyHow a speech therapist went from house visits to opening 3 locations using Tebra
Chimezie Chidi founded Celebrations Speech Group to deliver 1-on-1 sessions to clients
Read more -
 The Intake
The IntakeMedical insurance credentialing 101: Everything you need to know to avoid losing money and clients
From avoiding hours of paperwork to getting paid by insurance companies, find out what you need to know about medical insurance credentialing
Read article -
 The Intake
The IntakeClean medical claims: What you need to know for increased revenue
It’s not enough to just be proficient at submitting clean claims. Get the latest trends in medical claims submission from a medical industry expert
Read article
