Quality programs & regulatory support
Maximize reimbursements and earn positive performance-based payment adjustments.

Why Tebra?
Get higher MIPS scores and earn more with Tebra

Quality dashboard
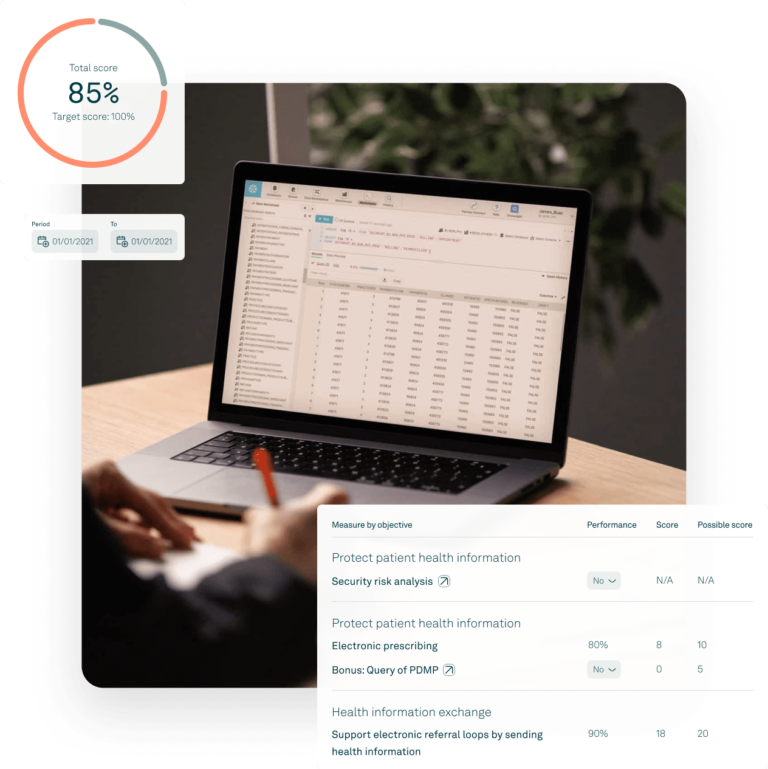
MIPS promoting interoperability dashboard

The Backbone
Visit our blog for helpful information about how to run a thriving practice, with topics including:
Frequently asked questions
-
What is MACRA?
MACRA is the Medicare Access and CHIP Reauthorization Act, which is legislation that replaced the Sustainable Growth Rate (SGR). It outlines a program for physician reimbursement that replaces fee-for-service with value-based payments under the Quality Payment Program (QPP).
-
What is the Quality Payment Program?
The QPP is the portion of MACRA that defines the value-based reimbursement system. It has two parts: the Merit-Based Incentive Program (MIPS) and Advanced Alternative Payment Models (APMs).
-
Who participates in the QPP?
The following provider types must participate in the QPP in either MIPS or APMs: physician (doctor of medicine or osteopathy, dental surgery or dental medicine, podiatric medicine, or optometry; chiropractor), physician assistant, nurse practitioner, clinical nurse specialist, clinical social workers, certified nurse midwives, certified registered nurse anesthetist, physical therapist, occupational therapist, clinical psychologist, qualified speech-language pathologist, qualified audiologist, and registered dietitian or nutritional professional.
-
Do I need a certified EHR to participate in the Quality Payment Program?
Yes, for both MIPS and the APMs, you need a certified EHR. The EHR must be 2015 Edition Cures Update certified.
-
Are there exceptions to the eligible provider?
Yes, there are two exceptions applications available to clinicians in the 2023 performance year: the Extreme and Uncontrollable Circumstances Exception and the MIPS Promoting Interoperability Performance Category Hardship Exception.


ONC Health IT Certification
This Health IT Module is compliant with the ONC Certification Criteria for Health IT and has been certified by an ONC-ACB in accordance with the applicable certification criteria adopted by the Secretary of Health and Human Services. This certification does not represent an endorsement by the U.S. Department of Health and Human Services.
-
Vendor Name: Tebra Technologies, Inc.
- Website: www.tebra.com
- Address: 1111 Bayside Drive, Suite 150 Corona Del Mar, CA 92625
- Contact: Beth Lyn Onofri, Sr. Product SME - Regulatory, [email protected], (866) 93-TEBRA (83272)
- Product Version: Tebra (Kareo) EHR v. 5.0
- Date certified: 12/19/2022 by Drummond Group, Inc.
- Certification No.: 15.04.04.2777.Tebr.05.02.1.221219
- Tested and Certified Modules: 170.315 (a)(1-5, 9, 12, 14); (b)(1-3, 10); (d)(1-9, 12-13); (e)(1, 3); (f)(5); (g)(2-7, 9-10)
- Additional Software Required: LabSoft, Updox, DrFirst Rcopia, SmileCDR
Cost and Considerations
The monthly subscription fee for Tebra (Kareo) EHR v 5.0 includes all tested and certified modules listed above with exception of a one-time small set-up for implementation of e-prescribing of controlled substances. For a detailed explanation of costs and guidance, click here. Optional services, which are not required for CMS Incentive Programs, are available for a nominal fee. These services include custom template development and private CMS Incentive Programs coaching.
Real World test plans:
| Year | Test Plan | Test Result |
| 2022 | 2022 Test Plan | 2022 Test Results |
| 2023 | 2023 Test Plan | 2023 Test Results |
| 2024 | 2024 Test Plan | |
| 2025 | 2025 Test Plan |
APIs
EHI Export Functionality
Tebra (Kareo) EHR enables providers to export out EHI for individual patients and their patient population at any time without developer assistance. Export formats include C-CDA documents for clinical records, PDFs for claims and billing information, and also documents in the original native format which they were uploaded.


